Pulmonary Fibrosis Diagnosis
It’s a different path for each individual which is why pulmonary fibrosis is so difficult to diagnose. It takes two years on average for patients to receive their pulmonary fibrosis diagnosis.

Early Detection is Key
Since it’s a rare disease, pulmonary fibrosis (PF) is not top of mind for most family practitioners. The 2022 CPFF Patient and Caregiver Survey highlights that many patients wait two or more years for a confirmed diagnosis.
PF symptoms cannot be reversed by the treatment medication, only slowed down. More awareness by the public and medical professionals can result in earlier diagnosis so treatments can start sooner for patients at a less severe stage of the disease.
Obtaining a Diagnosis
Patients with pulmonary fibrosis experience symptoms that are often subtle and similar to other lung disorders. For a pulmonary fibrosis diagnosis, a doctor will take a complete medical history and perform a thorough physical examination. During this examination, the doctor will listen to the patient’s chest to determine if their lungs are producing any abnormal sounds while breathing.
Types of pulmonary fibrosis
Once a doctor suspects pulmonary fibrosis, the next step is to try to diagnose the specific type of pulmonary fibrosis — there are more than 200 different kinds. Doctors typically start by asking questions, performing a careful physical examination, and ordering several blood tests.
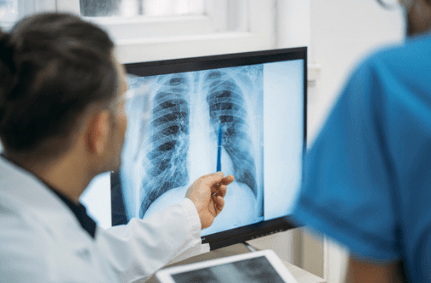
Chest Imaging
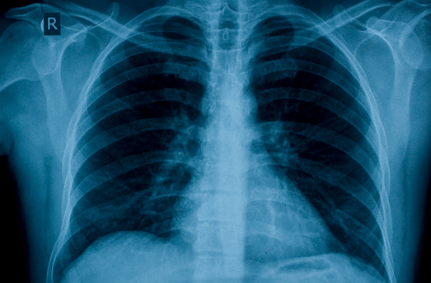
When looking for a pulmonary fibrosis diagnosis, this test helps the clinician view lung structures, look for scar tissue, and assess patterns of scarring.
Radiologic machines are used to take pictures of your lungs, such as x-ray or High-Resolution Computer Tomography (HRCT).
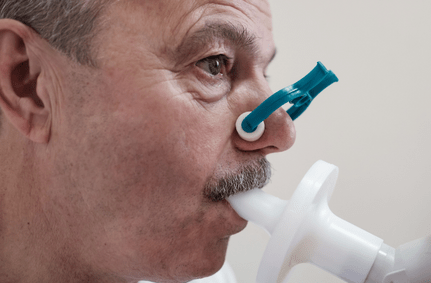
Pulmonary Function Test
Measures the degree of impairment in lung function using a device with a mouthpiece to measure a patient’s breathing capacity.
Exercise Test or Desaturation Study
When looking for a pulmonary fibrosis diagnosis, this test measures how well the lungs and heart respond to physical activity and evaluate oxygen levels with exertion by monitoring the patient while using a treadmill or stationary bicycle.

Six Minute Walk Test (SMWT)
Measures the distance a person can walk as well as lung function during the walk. During this test the patient walks on a flat surface as far as possible in six minutes.
Symptoms of Pulmonary Fibrosis
Tackle the Crackle© – Common Early Symptoms
Early detection is vital to slowing down the disease, so primary care professionals as well as all Canadians need to know PF can start with these common symptoms:
Persistent cough that won’t go away after more than 3 months
Shortness of breath after physical activity that was typically not a problem
Ongoing fatigue, weight loss
If you have any of these symptoms ask your Dr. to listen for the tell-tale lung crackles.
Ongoing PF Signs and Symptoms
Symptoms usually have a gradual onset and may include:






Pulmonary Fibrosis Looms Large for a Growing Number of Canadians
Many with long COVID-19 and connective tissue diseases are also more prone to PF
Research studies done across the world are shedding light on the growing rate of pulmonary fibrosis (PF) being found in people suffering from long-term COVID-19.

Tune in as Dr. Janet Pope shares what you need to know about interstitial lung disease (ILD) in connective tissue diseases.

The researchers also show significant increases in PF for the hundreds of thousands of Canadians suffering from connective tissue diseases such as rheumatoid arthritis, myositis, lupus and scleroderma.
More on Pulmonary Fibrosis Diagnosis
Genetics & ILD – Dr. Grant-Orser & Dr. Johannson
ILD respirologists Dr. Amanda Grant-Orser and Dr. Kerri Johannson discuss how genetics can be an important tool for patients with ILD, shared the results of a recent national patient survey, and explained genetic testing in Canada.
Navigating a New Pulmonary Fibrosis Diagnosis
In this webinar, Dr. Matthew Binnie discusses how to navigate a new pulmonary fibrosis diagnosis . Dr. Binnie is an Assistant Professor at the University of Toronto and Staff Physician at the Toronto Lung Transplant Program.
Better Pulmonary Imaging with Duel Energy X-ray
Learn how new Dual Energy X-ray technology can better detect, monitor progression, and speed up pulmonary fibrosis treatment.
Understanding Pulmonary Fibrosis: The Basics – Dr. Lawrence Homik
Tune in as Dr. Lawrence Homik, a community-based respirologist helps patients and caregivers understand the basics of pulmonary fibrosis.
Read Next…
Questions for Your Doctor
Asking the right questions when you meet with your doctor can empower you and help…
ILD Respirologists Across Canada 2024
This handout for people living with IPF and their families provides information on what idiopathic…
Research Studies: Post COVID-19 Pulmonary Fibrosis
Research is shedding light on the growing rate of pulmonary fibrosis (PF) being found in…
PF Patient Guide
Pulmonary Fibrosis Patient Guide (English) Guide du patient sur la fibrose pulmonaire (Français) – The…









