Oxygen Therapy
Supplemental oxygen can help you keep active and improve your quality of life.
Try to focus on all that supplemental oxygen can help you to continue doing, rather than seeing it as some kind of failure or focusing on the inconvenience.
Although it should be an effortless act, breathing for people with a lung disease like pulmonary fibrosis (PF) can be a painful, challenging experience.
It is common for people with PF to use supplemental oxygen, although not everyone needs it. Feeling breathless is a complicated process. Some people feel out of breath, but their oxygen levels are within the normal range. And some people won’t feel out of breath when their blood oxygen levels are too low (hypoxemia). Supplemental oxygen will only help you if your blood oxygen levels are too low.

Knowing when you need supplemental oxygen
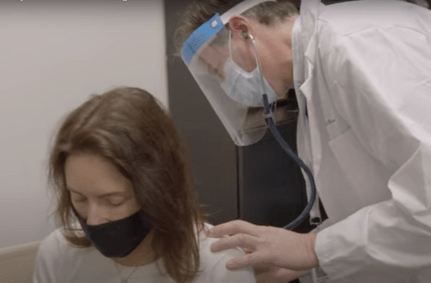
Your doctor will know if you need supplemental oxygen by doing tests such as the 6-minute walk test, arterial blood gases, and checking your pulse oximetry. You may need oxygen all the time, only with physical activity, or when you sleep.
You will be tested for your oxygen saturation; how much of the hemoglobin contains oxygen. It should be greater than 90 per cent at all times. Your physician will also test your arterial blood gases by taking a small amount of blood from an artery, usually the wrist. You may be tested while at rest and while walking. These tests will determine whether you qualify for oxygen therapy.
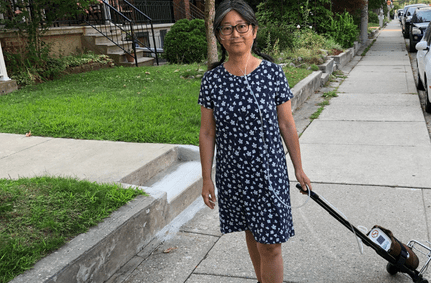
Oxygen therapy benefits
Supplemental oxygen will NOT cure your PF, however many people report that they have less breathlessness, fatigue and can live a more active lifestyle. Even if oxygen therapy does not take away your breathlessness, it can help you maintain proper blood oxygen levels which is important for your muscles, organs, and brain to function properly.
You cannot get addicted to oxygen. It is important to treat your oxygen as a prescription and use it exactly as your doctor prescribes.
Using oxygen therapy
It can take time to adjust to using supplemental oxygen. There are some things that might be more difficult with supplemental oxygen. For example, it may be more challenging leaving the house and carrying your oxygen, but newer models are increasingly light and portable. It can also make some things easier since you may experience less breathlessness, and you may get less tired doing activities.
There is some stigma associated with using oxygen in public. You may feel embarrassed. Try to focus on how oxygen therapy enables you to do the things you love, rather than consider it a failure or an indication that your disease is progressing towards the end. Explain to your family and friends how oxygen therapy helps you, to increase everyone’s comfort level.

Oxygen therapy systems
There are different types of machines that you can use to get supplemental oxygen. They are increasingly becoming lighter, more portable and easier to use. You will decide which option(s) is best for you with your doctor and your supplemental oxygen supplier.
Learn more about how supplemental oxygen equipment can be set up and used at home to help you go about your daily activities.
Oxygen Concentrator
For patients who are less mobile, an oxygen concentrator takes oxygen from the air in a similar way to how a dehumidifier takes water from the air. The device runs on electricity in your home so you usually need to have some spare oxygen tanks in case there is a power outage.
Portable Oxygen Concentrator (POC)
For more active individuals, depending on your prescribed oxygen flow rate, a portable oxygen tank may be used and can last up to a few hours. Your doctor will determine what dose is sufficient to maintain a normal blood oxygen level during your usual normal daily activities at home and away.
Oxygen Storage Pendant
Reduces the oxygen supply flow necessary to achieve adequate oxygen levels. It requires the use of a reservoir designed like a necklace, away from the face and hidden from view by the patient’s clothing.
Long Oxygen Tubes with Canula
To assist with your mobility at home, patients may find it is beneficial to have an oxygen tube at home as long as 50 feet. This will give you the ability to move around without dragging a portable tank with you all the time.
- If you live in a smaller space, this length of tubing may not be necessary. The length of tubing should allow you to move around high traffic areas of your home without having to carry your oxygen tank with you.
- If you have a two-story home with your bedroom upstairs, you may want a second tube in your bedroom long enough to reach the bathroom.
Although traveling can be tiring if you have PF, there is no reason to stay at home while others take vacations, visit family, or travel for business. Even if you are on supplemental oxygen, with proper advance planning, you can travel safely.
Planning for Travel with Supplemental Oxygen
Traveling with supplemental oxygen may mean that you encounter some extra challenges, but with planning, you can be comfortable and safe on the road or in the air. Also check if your final destination has medical oxygen available.
Ensure you have travel insurance if visiting the United States, as medical costs there can be extremely expensive.
As a Canadian citizen, you have health coverage for travel anywhere in Canada.
- If you use supplemental oxygen, plan travel in advance
- Work with your healthcare team to improve your breathing ability
- Check with your doctor to make sure it is safe for you to travel
- Decide how you will be most comfortable traveling; by car, bus, train, plane, or ship
- If your destination is at a high elevation, ask your doctor about additional oxygen needs
- Ask your doctor for a letter stating the medications you are on and take your original prescription bottles with you
- Always carry a list of the medications you are taking in case of an emergency
Ground Travel
While some people load the car with their oxygen tanks and make road trips, others prefer the comfort of a train or bus.
Travel requirements change frequently on trains or buses, so check with your carrier for the latest and most accurate information.
- Make reservations as far in advance as possible
- Speak with someone in Customer Relations when making reservations
- Do not depend on on-board electrical power
- For longer trips, plan for a 12-hour, backup oxygen that does not require electricity
- If transporting your oxygen by car, be aware of safety issues
- Bring enough oxygen for the length of your trip, plus 20 percent extra to allow for delays
Air Travel
Each airline has different rules that can change at any time.
Click here for Air Canada’s travel tips for travelling with oxygen.
You may be required to provide a doctor’s statement of your ability to travel and of your oxygen needs before you will be allowed to take or use oxygen on a commercial airline flight.
- Contact the airline as far in advance as possible
- Speak to airline’s special services
- As about bringing your own oxygen equipment
- If you must use airline‐supplied oxygen, ask about the cost
- Airlines often do not provide oxygen for use in terminals; if you must change planes, you may need to make other arrangements
- Call your current oxygen provider; they may be able to provide helpful information
- For more information, contact your travel agent or airline directly
More on Oxygen Therapy
Oxygen 101 with VitalAire
Get informed about oxygen therapy with this Oxygen 101 webinar featuring respiratory therapists from VitalAire – Kelsey Kress and Natalie Collins.
Jeannie Tom’s Pulmonary Fibrosis Journey
Jeannie Tom is limited by what she can do when tethered to an oxygen tank. It takes careful planning to go about her day. Learn about Jeannie’s PF journey and the many ways she manages her disease.
A Patient’s Journey with Oxygen – Ron Flewett
Oxygen and Interstitial Lung Disease (ILD)
Read More…
The Harvey family had to move to Ontario for Eileen Joyce to get the care and liquid oxygen she needs
When Eileen Joyce Harvey was 58 years old, she packed up to head for Toronto…
Home Delivery of Liquid Oxygen Not Available to PF Patients in Most Parts of Canada
Each province and territory have different funding programs for home oxygen therapy and unless you…
Access to Oxygen Therapy in Canada Reports
Learn what PF patients, health care pros and oxygen providers are saying about Oxygen in…
Oxygen Therapy Frequently Asked Questions
These Oxygen Therapy FAQs from ProResp provides tips for safely using oxygen at home and…
Making a Case for Oxygen Therapy Survey
Learn about the results of a survey conducted by Dr. Kerri Johannson of the University…
How to Access Oxygen Therapy in Canada
Learn about the requirements necessary to access supplemental oxygen coverage under federal and provincial programs….







