2024 Newsletters

April 2024
Our April Newsletter is out! Get the latest updates on new Robert Davidson fellows, insights on liquid oxygen, and an opportunity to celebrate the …

March 2024
CPFF March Newsletter is here! Meet new CPFF staff, learn about chronic cough research, Rare Disease Campaign activities, advocacy initiatives, and more …

February 2024
The Canadian Pulmonary Fibrosis Foundation (CPFF) is pleased to announce the appointment of Todd Georgieff as Chair of its Board of Directors during the …
2023 Newsletters

December 2023
A message from our outgoing Board Chair After six years of volunteer service as the CPFF Board Chair, Kirk Morrison will be leaving the …

November 2023
You did it! Participants gather for a photo at the Khan Family Walk for PF during Pulmonary Fibrosis Awareness Month in September. We all …

October 2023
Breathing has to be a fundamental human right and equal for all Canadians CPFF has surveyed patients, caregivers, health professionals and oxygen providers to …

September 2023
Embrace hope this September These participants are having their photo taken “on the farm” before the “Avonmore Run the Farm for PF,” last month …

August 2023
CPFF Robert Davidson Fellowships fill a gap in ILD care After completing several research projects, Dr. Amanda Grant-Orser has finished her two-year CPFF Robert …

June 2023
A unique case sparks a passion for ILD research and patient care Dr. Bohyung Min is just completing her one-year CPFF Robert Davidson Fellowship …

May 2023
CPFF research investment surpasses $2 million CPFF is pleased to announce the two Robert Davidson fellowships for 2023-24. Dr. Kirsten Nesset, above, will be …

April 2023
Today is National Caregiver Day Every person’s journey with PF is different, and so are the experiences of their family caregivers. Below are the …

March 2023
Developing clarity in CT scan analysis for better PF diagnosis Dr. Daniel Marinescu completed a two-year, CPFF Robert Davidson Fellowship, last summer, and will …

February 2023
People with rare diseases deserve equal access to health care CPFF is part of the global campaign to raise awareness of rare diseases and …
2022 Newsletters

November / December 2022
CPFFs 2022 Pulmonary Fibrosis Awareness Month campaign wrapped up at the end of September. And once again, our joint efforts have achieved great results …

October 2022
CPFFs 2022 Pulmonary Fibrosis Awareness Month campaign wrapped up at the end of September. And once again, our joint efforts have achieved great results …

September 2022
It’s Pulmonary Fibrosis Awareness Month! While events and activities are well underway, it’s not too late to get involved in Pulmonary Fibrosis Awareness Month …
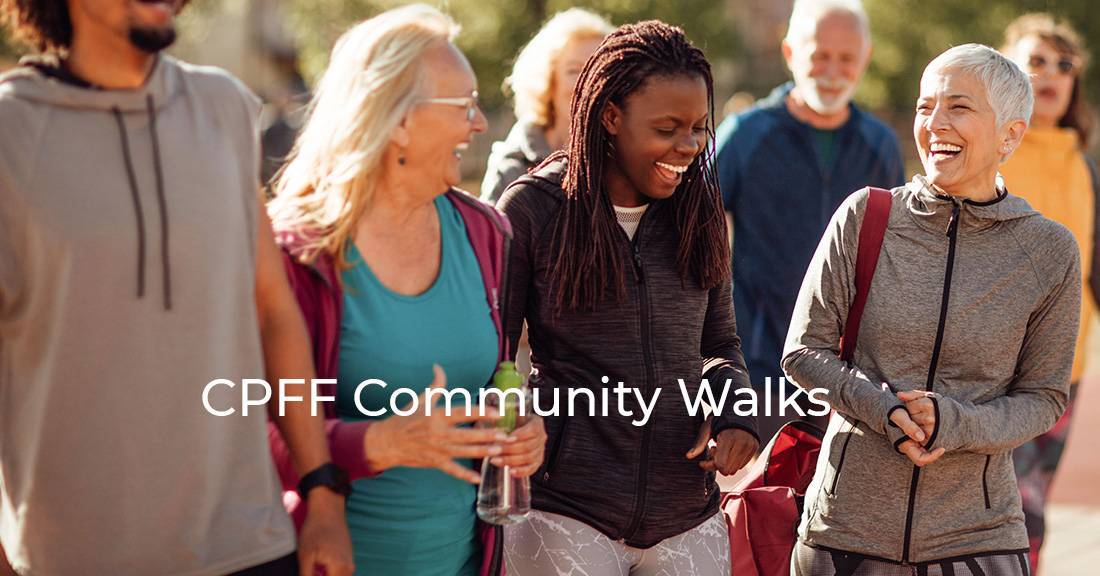
August 2022
Set up your own event, or support someone else’s, during Pulmonary Fibrosis Awareness Month in September. Whatever the challenge, Canadian Pulmonary Fibrosis (CPFF) supporters …

June 2022
CPFF’s 2022 patient and caregiver survey is open for your responses until this Friday, June 10. Don’t miss this opportunity to share your experiences …

May 2022
CPFF announces 2022-2023 Robert Davidson Fellowships Advancing research and developing more respiratory specialists to improve care, as well as expand access to care, for …

April 2022
Help us get nintedanib for all who need it We are very pleased to share the news that Alberta became the first province on …

March 2022
Celebrating rare individuals We are all unique individuals tied together by our dedication to a better life for people living with pulmonary fibrosis (PF) …

February 2022
Let’s breathe hope into 2022 A message from Sharon Lee, Executive Director, CPFF For our first issue of Hope Breathes Here in 2022, I …
2021 Newsletters

December 2021
Hope breathes here A message from CPFF Board Chair Kirk Morrison This has been another very challenging year as we dealt with the continued …

November 2021
Upcoming webinar explains new x-ray technology that may detect PF earlier We know that one of the biggest challenges of pulmonary fibrosis is obtaining …

October 2021
Thank you one and all! Despite the continuing restraints of a second year of the pandemic, this year’s virtual Pulmonary Fibrosis Awareness Month campaign …

September 2021
Enjoy the benefits of getting involved in Awareness Month activities September is Pulmonary Fibrosis Awareness Month around the world, and the Canadian Pulmonary Fibrosis …
August 2021
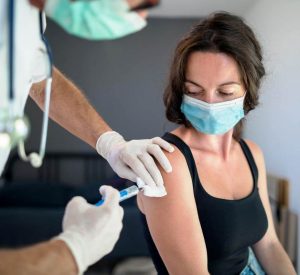
You are fully vaccinated against COVID-19. Now what? By now, we hope that most Canadians living with pulmonary fibrosis have been fully vaccinated, along …

June 2021
CPFF awards two Robert Davidson Fellowships The CPFF Board of Directors and Medical Advisory Board is pleased to announce two Robert Davidson Fellowships for …

May 2021
May, 2021 CPFF Fellow makes substantial contributions to ILD research In addition to caring for COVID-19 patients at Toronto General Hospital (TGH) for a …

April 2021
Anti-fibrotic drugs and the COVID-19 vaccines and a new vaccine webinar The Canadian Pulmonary Fibrosis Foundation (CPFF) has reached out to the appropriate pharmaceutical …

March 2021
Get vaccinated as soon as you can The Canadian Pulmonary Fibrosis Foundation has been receiving many inquiries from individuals with PF and their carers …

February 2021
Barbara Barr-Haylock was a champion of knowledge for people with PF It is with great sadness that the Canadian Pulmonary Fibrosis Foundation (CPFF) Board …

January 2021
Reflecting on 2020 As the new year begins, I am spending time thinking about the gratitude, regard and appreciation of the pulmonary fibrosis (PF) …
2020 Newsletters

August 2020
We may be vulnerable, but we are also strongBy Sharon Lee, Executive Director, CPFF As Canada’s largest cities and smaller towns enter stage three …

December 2020
Message from CPFF Board Chair, Kirk Morrison Kudos to Kirk Mathison for a great Calgary Support Group meeting on December 1! More than 50 …

November 2020
Resources to help you through the second wave of COVID-19 As people have been heading back to work and school this fall, the second …

October 2020
I’ve been diagnosed with pulmonary fibrosis… Now what? For anyone newly diagnosed with pulmonary fibrosis or their family member, Dr. Charlene Fell’s webinar is …

September 2020
Make connections and enjoy September By Kirk Morrison, Chair, CPFF As we all know, September is Global Pulmonary Fibrosis Awareness Month. In a year …

June 2020
Message from the Board Chair Kirk Morrison Just thought I would let everyone know, that despite the pandemic, the CPFF Board of Directors have …

May 2020
May, 2020 New resources answer your questions about PF and COVID-19 CPFF has two new webinars, featuring expert speakers, to help you manage during …

April 2020
A Message from the Executive Director Dear Pulmonary Fibrosis Community, I want to start by offering my sincere thanks and appreciation to all of …

March 2020
Study gives researchers a first overview of PF in Canada A recent study of 1,285 patients, older than 18, who enrolled in the Canadian …
2019 Newsletters

May 2019
Founder Robert Davidson leaves a legacy with CPFF Robert Davidson, CPFF Founder It is with great sadness that we announce the passing of Founder …

April 2019
Advocating for you Sharon Lee, Executive Director, CPFF meets with MPP John Fraser With a new government in Ontario, CPFF has been busy this …

March 2019
A Message from Kirk Morrison, CPFF President: All,It’s hard to believe that we’re drawing near the end of the first quarter of 2019! I’ve …

December 2019
New report reveals major gaps in care for Canadians with IPF The current state of care for Canadians living with idiopathic pulmonary fibrosis (IPF) …

November 2019
Study investigates the association between muscles and ILD A recent UBC study of 115 people with Interstitial Lung Disease (IDL), including 40 people with …

October 2019
Exploring the mysteries of the cellular pathways to fibrosis A recently completed study by Dr. Kjetil Ask and PhD student Olivia Mekhael sheds new …

September 2019
Message from the President Hard to believe that the summer is over, and that Pulmonary Fibrosis Awareness Month is kicking off! Not sure if …

August 2019
Two research grants announced The Canadian Pulmonary Fibrosis Foundation is pleased to announce two, $20,000 research grants for 2019-2020 and gratefully acknowledges the Parkash …

June 2019
CPFF research funding totals more than $1 million The Canadian Pulmonary Fibrosis Foundation’s research investment total tops $1 million with the funding of two, …



